Contributed by Mark Callanen, PT, DPT, OCS and Perry Nickelston DC, NKT, FMS, SFMA
Osteoarthritis (OA) is a debilitating joint condition that effects more than 27 million individuals in the United States.1 According to the Centers for Disease Control and Prevention (CDC), 80% of patients with OA have some limitation of mobility, while 25% are unable to perform the activities of daily living (ADLs)2. Osteoarthritis is thought of as “wear and tear” arthritis and is caused by prolonged, abnormal stress on joints that leads to the breakdown of cartilage on joint surfaces. This is often associated with increased pain while performing daily activities.
When OA pain flares, people often become desperate for relief when they find themselves unable to tolerate the physical demands of a normal day. Many arthritis sufferers often see medication as the only option to alleviate their symptoms. This is part of the reason excessive opioid use has become a national health epidemic. While medication plays a part in most treatment plans, there are other activities and treatments that arthritis sufferers should consider when trying to manage the pain associated with OA.
Closed Chain Exercises
Loosely defined, closed chain exercises are activities that are performed with the feet on the ground. Examples would be squatting or sit to stand activities. Some people suffering from OA in their lower extremities are afraid of weight bearing because of the pain they are experiencing. However, when done properly, this is exactly what is needed.
Small amounts of weight bearing exercise performed over 3 months might not change the volume of cartilage in the knee, but it can significantly reduce pain and improve functional levels.3 This is because even when a joint is considered “arthritic”, exercises like squatting and wall slides can help strengthen the muscles around the joints of the hip, knee, and ankle. This can help improve the biomechanics of how a person is moving and reduce their pain.
Other studies have shown that people committed to exercising for 4 months or longer, focusing on exercises that cyclically load the legs three times a week, can increase the production of cartilage in the knee.4 Setting yourself up with a program that stresses the legs, but isn’t too aggressive, stimulates the cartilage to produce chemical changes that retain more water and thicken.4 This can make the difference between function and failure. Working with a trained professional to get a safe, pain free exercise regimen is imperative to incorporating the correct exercises into your program.
Stretching
Another important fitness component to helping with arthritic pain is making sure that normal muscle length is maintained throughout the body. Lack of stretching can lead muscles and tendons to become morphologically shortened, which increase the probability they will contribute to pain around the joint. The last thing an arthritic joint needs is to be surrounded by soft tissue that is inflamed and irritable. Staying proactive with a regular stretching regimen should help minimize the chances of this happening.
Stretching can directly promote joint health when it restores normal range of motion. People with OA often have reduced knee ROM which can be due to numerous factors. 5 When joints move, the various surfaces of the joint contact each other which is needed for cartilage to remain healthy. When joints get stiff or if muscles are tight, often the resultant loss of motion does not allow all of a joint’s surfaces to be stimulated. This can lead to cartilage break down. The best defense against this is to keep joints moving through their full ranges.
Aquatic Therapy
For those individuals that have more severe OA, they might not be able to bend or squat effectively against gravity due to pain. A pool allows exercise to be conducted in a partial weight bearing environment, which can be a great bridge to help increase strength and endurance. The buoyancy of the water decreases the forces that are transferred to the legs when contacting the bottom of the pool and the hydrostatic pressure of the water helps reduce pain in arthritic joints.
Generally, when standing in waist deep water, body weight is reduced by 50%. When standing in water at chest height, relative body weight drops to 25%. Participants want to gradually migrate to shallower water as their program progresses to increase the percentage of weight bearing with activity. The eventual goal is to try to transfer the program to land-based as tolerated. Seeking out an experienced aquatic therapist to help build and progress a water based program is a great place to start.
Deep Tissue Laser Therapy
In addition to actively addressing fitness levels, deep tissue laser therapy offers an effective passive treatment option that can help reduce arthritic pain. The pain and inflammation that occur in the majority of the body’s joints is created by inflammation of the tissue lining the joint capsule. Therapeutic laser can impact this tissue by improving the microcirculation in the tissue and impacting several anti-inflammatory mediators in the joint. Pain is normally reduced when these changes take place.
In addition to the metabolic effects laser has on inflamed tissue, it also provides a soothing warmth during treatment which also helps the body relax. Individuals will often feel a significant improvement from the first session. While each case is unique, typical treatment protocols call for 6-10 sessions for optimal results, and treatments are often short (about 5-10 minutes in length).
Here’s an example of how these approaches can be combined to minimize pain in an arthritic knee:
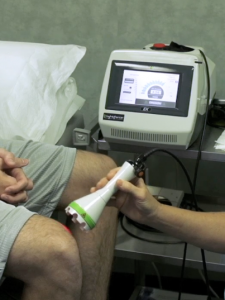 Laser therapy: apply deep tissue laser therapy to the knee joint, calf, lower thigh and lumbar spinal nerves 3-5 at 10 watts of power for 7 minutes (4500 joules total). Better outcomes have been recorded when recipients actively move the joint being treated during 40-50% of the treatment duration in that area. Motion ensures that light reaches all aspects of the treatment area and encourages better range of motion in the affected joint.
Laser therapy: apply deep tissue laser therapy to the knee joint, calf, lower thigh and lumbar spinal nerves 3-5 at 10 watts of power for 7 minutes (4500 joules total). Better outcomes have been recorded when recipients actively move the joint being treated during 40-50% of the treatment duration in that area. Motion ensures that light reaches all aspects of the treatment area and encourages better range of motion in the affected joint.- Stretching: spend 5 minutes stretching the knee by fully bending and straightening it while standing next to a stable object. Hold stretches for 15 seconds, rest, and repeat for approximately 2 minutes per muscle to be stretched. Additional stretches at the ankle to promote dorsiflexion and hips to promote motion in multiple planes is recommended. Specific stretching techniques should be provided by a trained professional.
- Closed chain exercises: spend 10-15 minutes working on sit to stands, squats, wall slides, and some type of step up exercise to help build strength in the lower extremities. They should not be painful. Again, specific exercise techniques should be provided by a trained professional to match the program to an individual’s specific functional ability.
- For those individuals that cannot perform a land based program, substitute an aquatic program to work on strength and endurance for 20-30 minutes.
You can take back control of your life from the pain and discomfort of arthritis. Empower yourself to feel good again with movement, stretching, and laser therapy. While the idea of stretching and strengthening isn’t ground breaking, combined with the unique capabilities of deep tissue laser therapy, it might just be your ticket to lasting relief.
1. Leahy M. Changing the paradigm for diagnosing and treating arthritis. American Academy of Orthopaedic Surgeons. http://www.aaos.org/news/ aaosnow/nov12/clinical6.asp. November 2012. 2. Centers for Disease Control and Prevention. Arthritis basics. Physical activity for arthritis. http://www.cdc.gov/arthritis/basics/physical-activityoverview.html. September 1, 2011. Updated January 7, 2016. 3. The effects of closed kinetic chain exercise on articular cartilage morphology: myth or reality? a randomized controlled clinical trial. Dinçer U et al. Turk J Phys Med Rehab 2016;l(62):28-36 DOI: 10.5606/tftrd.2016.93899 4. Roos EM, Dahlberg L. Positive effects of moderate exercise on glycosaminoglycan content in knee cartilage: a fourmonth, randomized, controlled trial in patients at risk of osteoarthritis. Arthritis Rheum 2005;52:3507-14. 5. Dieppe, P. Osteoarthritis: time to shift the paradigm. British Medical Journal, 1999; 318, 1299-1300



