Laser Therapy FAQ 4 – If Lower Doses of Laser Light Can Help Tissue Heal, Then Why Would I Need More Power?

Contributed by Mark Callanen, PT, DPT, OCS
Unlike in the movie Spinal Tap, where having an amplifier that “goes to 11” doesn’t mean it’s actually going to be louder than any other amplifier, having a laser with higher power will enable you to do things a much lower power laser will not. Looking into a Class IV laser (one that has over 0.5 W of power) is a wise investment if you are planning on putting a laser in your clinic.
The biggest challenge with low level laser therapy (LLLT), more correctly referred to as photobiomodulation therapy, is getting light energy in sufficient quantity to injured tissues. Skin does an excellent job scattering and reflecting most of the light that it is introduced to it. Additionally, melanin absorbs most of the remainder of light into the skin, leaving very little to get transmitted below skin level. When normal white light or sunshine hits the skin, very few photons get past this impressive gate keeper.
Certain wavelengths of light energy penetrate the skin better than others. Unfortunately, additional barriers exist under the skin that want to grab or reflect more of the remaining light that gets past the skin1. These include hemoglobin, oxyhemoglobin, fat, and water to name a few. Therefore, careful consideration has to be given when choosing therapeutic wavelengths to maximize a laser’s effectiveness on influencing the healing process of muscle, nerve, tendon, and other connective tissue.
Wavelengths around the near infrared portion of the spectrum (800 to 1000 nm) are ideal for exciting chromophores in tissue under the skin and not getting absorbed by the obstacles previously listed2. Even when using ideal wavelengths, there is a significant loss of light energy from the surface to only a few centimeters below the skin. Rabbit studies have confirmed that only 2-3% of surface light reached the peroneal nerve when applied on shaved skin3.
As if the natural barriers to light weren’t enough, most injuries involve dozens to hundreds of square centimeters of tissue damage. When larger areas need to be treated, even more power is needed at the surface to maintain the same therapeutic dose at depth over the entire treatment area2. Therefore, even if you are using a laser that has the appropriate wavelengths to penetrate tissue ideally, but has a very low level of overall power, you will only be able to effectively treat very small areas. Additionally, treatments may take 30 minutes or longer to get it done2!
A review of how power and time relate to the overall joules applied to an area will help clarify this problem. Laser dosage is defined as joules/cm2. It is a function of (wattage x time)/ area. If a laser has low power (wattage) and/or you need to treat a large area, these two factors can only be overcome by significantly increasing treatment time to maintain the desired dosage.
This is the plight of Class IIIb lasers and is a primary reason a lot of early laser research had underwhelming outcomes. Insufficient dosage to injured tissue will not affect significant change at the mitochondria, and the positive effects of photobiomodulation will not be realized.
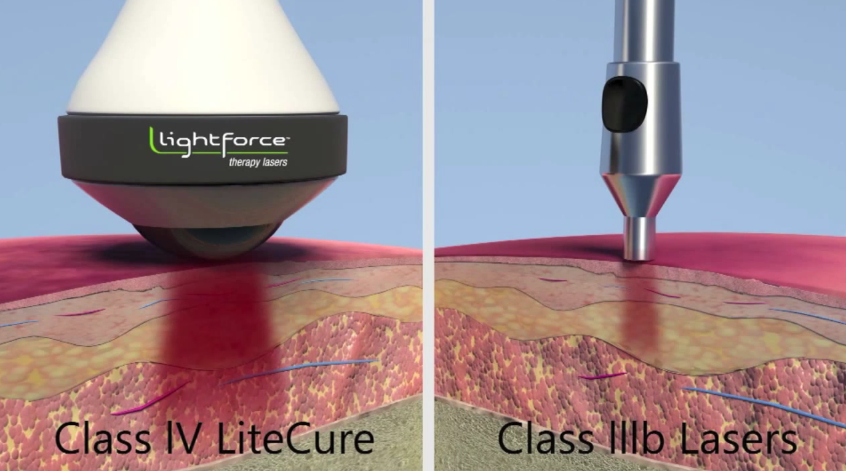
This concept helped influence the FDA in 2004 to accept the use of Class IV lasers for photobiomodulation. Class IV lasers start where Class IIIb leave off at 0.5W of power. This higher wattage allows for sufficient laser energy to be passed onto nerve, muscle, ligament, tendon, and/or capsular tissue in a reasonable amount of time. Normal treatment sessions range from 2-6 minutes, which is quite acceptable in a clinical setting. Higher powered lasers will also allow clinicians to have the versatility to treat injured tissue in multiple areas in a given session, which greatly improves the overall effectiveness of the laser when adding it to a plan of care.
Class IV lasers are generally more expensive than Class IIIb technology, but there is no real comparison when it comes to clinical application. “You get what you pay for” is applicable here. Other factors to consider when comparing laser products include: where the device is manufactured, warranty parameters, application heads, and what type of customer service is available to help educate your staff on how to effectively use the laser after it is purchased.
While cost is an important variable with any purchase, careful consideration should be given to these factors as well as how you intend to use the laser. Getting a device that best fits your patient population and your clinic’s budget will help create a win-win for your patients and your facility from whichever laser platform you decide to purchase.
1. Hamblin MR, Demidova TN. Mechanisms of low level light therapy. Proc. of SPIE Photonics. 2006; 6140: 614001-01-12. doi: 10.1117/12.646294 2. Chris E. Stout, Matt Kruger and Jeffrey Rogers, (Eds)- © 2011 Bentham Science Publishers Ltd. Current Perspectives in Clinical Treatment & Management in Workers’ Compensation Cases, 2011, 15: 191-201. 3. Anders JJ, Bethesda, MD. In Vitro and In Vivo Optimization of Infrared Laser Treatment for Injured Peripheral Nerves. Lasers Surg Med. 2014 Jan;46(1):34-45. doi: 10.1002/lsm.22212. Epub 2013 Dec 11.
Comments