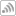Next to its unique characteristics allowing patient stress, fear, and pain to be reduced, photobiomodulation therapy (PBMT) also has the ability to be utilized as an adjunct to standard of care for a myriad of conditions affecting species ranging from the smallest avian to the biggest elephant. PBMT offers us not only a noninvasive and painless tool, but it also affords the operator certain flexibility in its applications, as per the level of tissue disruption involved.
Next to its unique characteristics allowing patient stress, fear, and pain to be reduced, photobiomodulation therapy (PBMT) also has the ability to be utilized as an adjunct to standard of care for a myriad of conditions affecting species ranging from the smallest avian to the biggest elephant. PBMT offers us not only a noninvasive and painless tool, but it also affords the operator certain flexibility in its applications, as per the level of tissue disruption involved.
Certainly, each case is an individual instance and must be approached with an individual treatment design and delivery plan. Just as no two patients are the same, neither are the specifics surrounding the etiology / progression / current status and treatment care / etc. of each case. PBMT offers us the flexibility of addressing cases where there is any level of pain, inflammation, and/or tissue disruption. Most, if not all the patients we see, regardless of species, are likely to fit the bill in at least one of the three categories cited. Let’s take a look at some of the commonly-used ways in which a clinic can implement a successful PBMT program as an adjunct to standard of care.
Typically, a new adopter the modality will begin by using it for cases responsive to a short treatment course. Usually, these include acute conditions involving superficial tissues, such as pyotraumatic dermatitis and post-operative incisions. Naturally, as the operator’s knowledge base grows, so will the daily applications of the modality. Most operators report a positive experience in delivering this level of care. It is as therapeutic for the operator to provide this leading-edge level of care as it is for our patients to undergo it. The most challenging part of starting a successful and multifaceted PBMT program in a clinical setting is to overcome inertia. Once the ball gets rolling, it will naturally pick up speed.
 Once the operators have applied the early stages of making PBMT a core part of their multimodal approach to pain management, then the next natural evolution is to incorporate it with routine anesthetic procedures. Here, we see patients undergoing either a surgical or dental health procedure. In this setting, the therapy laser platform can again be utilized in a series of ways, from conditions such as gingivitis (the only reversible dental disease), going all the way up to multiple extraction sites or stomatitis. With surgical procedures somewhat more involved, like an extracapsular cruciate repair, a pre-op and post-op treatment would also prove to be of value. PBMT should also be highly considered as part of a convalescent care plan, especially when dealing with invasive or orthopaedic procedures (e.g. – FHO, TPO, TPLO, TTA, limb amputation, etc).
Once the operators have applied the early stages of making PBMT a core part of their multimodal approach to pain management, then the next natural evolution is to incorporate it with routine anesthetic procedures. Here, we see patients undergoing either a surgical or dental health procedure. In this setting, the therapy laser platform can again be utilized in a series of ways, from conditions such as gingivitis (the only reversible dental disease), going all the way up to multiple extraction sites or stomatitis. With surgical procedures somewhat more involved, like an extracapsular cruciate repair, a pre-op and post-op treatment would also prove to be of value. PBMT should also be highly considered as part of a convalescent care plan, especially when dealing with invasive or orthopaedic procedures (e.g. – FHO, TPO, TPLO, TTA, limb amputation, etc).
As with anesthetic patients, hospitalized patients should be given specific consideration and be offered the benefits of PBMT, especially while they are on location. Such examples that have shown the value of PBMT to standard of care include pancreatitis, HBC, degloving injuries, and snakebites, just to name a few. Typically speaking, “time is tissue” when it comes to injury to tissues (both soft and dense). The savvy laser operator is able to embrace this concept and thus understands to have a certain window of fluidity in the application of the modality. The operators’ knowledge base in PBMT and ability to be flexible with an in-patient approach treatment design and delivery, enables them to best address the individual needs and caveats of each case as a separate application (i.e. special considerations such as: active hemorrhage, neoplasia, or active growth plates).
Once a practice has reached this level of understanding and has applied a level of commitment in incorporating PBMT with their core values and message, and confident in its application, the final step is to incorporate it with long-term care plans. In this setting, the focus is on outpatient appointments, scheduled much as they would be for a DVM seeing outpatients. These are the long-term patients with incurable conditions where our goal (and reasonable expectation) is to manage the condition and prevent an active decline. Often, once a clinic gets to this level of focused care, a specific “daily designated laser operator” is usually assigned to the task of handling the daily appointments (larger practices with a sizeable technical staff will incorporate a rotation of daily operators so as to have everyone remain proficient in their technique).
Most practices successful in their integration and implementation of PBMT within their departmental daily modus operandi, in addition to the current standard of care, have proven the modality a synergistic behemoth in our ability to continue to adapt to, adopt, and successfully implement a dynamically evolving aspect of veterinary medicine. The successful and practical applications of PBMT are limited only by the specifics of the case and the ability of an operator to perceive the modality’s application for a specific case presentation. The initial inertia previously mentioned is quickly overcome and replaced by a momentum which will help propel any practice to the next level of patient care when PBMT is allowed to fully develop as a medical modality in clinical practice.